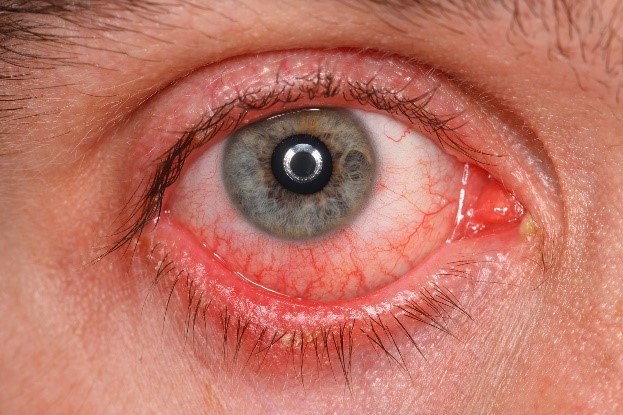
Corneal and external eye disease encompasses a very diverse range of conditions which can involve the cornea and its many layers, the endothelial, iris, lens, the conjunctiva, and eyelids. The cornea can sustain damage through foreign objects, abrasions and infections, edema (swelling), and scarring. The cornea can also be damaged through genetic or degenerative disorders. conjunctivitis (pink eye), dry eye, keratoconus, pterygium, Fuchs’ Dystrophy, cataracts, nearsightedness, farsightedness, and astigmatism are a few of the maladies that can affect or injure the cornea and conjunctiva.
Corneal Ulcers: Bacterial, viral, fungal and parasitic infections can occur when not exercising proper contact lens care, or failure to use protective eyewear at work or play. Corneal ulcers (open sores on the cornea) can be a result in these eye infections. Severe dry eye, eyelid disorders or contact lens misuse can cause ulcers as well.
Treatment: Antibiotic, antiviral or antifungal eye drops are the first line of treatment. Undiagnosed ulcers can also result in scarring of the cornea which may lead to surgical intervention. See your ophthalmologist at the first signs of pain or redness in the eye, severe pain or soreness, swelling of the eyelids, pus or discharge from the eye or white spots developing on your cornea. Do not try to self-medicate with over the counter drops unless directed by a physician.
Herpes Simplex Virus: There are two types of herpes simplex virus that affect the eyes commonly known as Type I (HSV I) and Type II (HSVII). Type I, the most common, is the same virus that causes cold sores and fever blisters and the viral infection can be caused by touching a cold sore and then touching or rubbing your eyes. Type II is spread through sexual contact. The infection once spread to the eye can spread deeper into the cornea causing redness and swelling and possibly the scarring of the cornea or ulcers on the cornea.
Treatment: There is no cure for ocular herpes. Once you have the virus, it remains in your body, but mild cases can often be controlled with antiviral pills and/or steroid drops. Your ophthalmologist may also scrape diseased cells from your cornea to help improve vision. If your cornea is scarred from a severe infection you may require a corneal transplant.
What is dry eye?
Normally, the eye constantly bathes itself in tears. By producing tears at a slow and steady rate, the eye stays moist and comfortable. Sometimes people don’t produce the right quality or quantity of tears to keep their eyes healthy and comfortable. This condition is known as dry eye.
Symptoms of dry eye: Stinging, burning, a scratchy or gritty feeling, strings of mucus in or around your eyes, pain when wearing contacts or, oddly enough, watery or excessive tearing are all symptoms of dry eyes.
How the tears work?
Your eyes produce and need tears to stay moist and healthy. When a person blinks, a film of tears is spread over the surface of the eye. This tear film consists of three layers: each layer has a special purpose.
An oily layer (Lipid) made in the Meibomian glands is the outside layer and keeps our tears from drying or evaporating too quickly.
A watery layer (Aqueous) produced by the lacrimal glands in the eyelids is the middle layer of tear film. This watery layer is what we commonly call tears and cleans and washes the eye.
The mucus layer (Mucous) helps to stick the watery layer or tears to the surface of the eye, in turn, keeping the eye moist. It is the innermost layer of the tear film. The conjunctiva or clear tissue that the covers the white of the eye and inside the eyelids produces the mucus.
The eye uses two speeds of production to produce tears. Either at a slow, steady rate to maintain normal eye lubrication or if irritated, or, for instance, we cry, at a much faster rate of production. Watery eyes, are a result of the eyes attempting to produce enough tears to correct the irritation that is disrupting the normal steady rate and therefore, a symptom of a dry eyes.
Causes of Dry Eye: There are many causes of dry eye. As we age, hormonal changes cause us to make fewer tears. This is more common in women who are post-menopause but can affect men as well. Diseases, certain medications, contact lenses, refractive surgery, long periods of reduced blinking while at the computer, dry, windy climates and other eye conditions can all contribute to dry eyes. Your ophthalmologist will want to know about all prescription and non-prescription you take and will do a thorough exam before deciding on your treatment plan.
Treatment: Depending on the cause and severity of your dry eye condition and after a thorough discussion with your ophthalmologist a treatment plan will be developed. This generally falls into the following categories:
- Increasing Tears – You may be given a prescription for eye drops that aid in tear production
- Adding Tears – Artificial tears may be recommended which can be purchased over the counter.
- Saving Tears – Punctual Plugs may be recommended to block your tear ducts enabling your natural tears to remain in and on the eye longer. These plugs can be removed later as needed or surgery may be recommended to permanently close your tear ducts.